Activities of Daily Living (ADLs): Practical Guide to Assessment & Care
Who handles the simple tasks in daily life—bathing, dressing, eating—can tell you a lot about a person’s independence. Those tasks are called activities of daily living, or ADLs. Knowing what ADLs are and how to check them helps you care smarter, plan safer homes, and talk clearly with doctors and therapists.
What ADLs Are and Why They Matter
ADLs are basic self-care tasks everyone does every day. The common list includes: bathing, dressing, toileting, transferring (like getting in and out of bed or a chair), continence, and eating. If someone struggles with one or more ADLs, they may need help at home, equipment, or therapy. That affects safety, mood, and health costs.
There’s also a second group called IADLs—instrumental activities of daily living—like cooking, shopping, managing money, and driving. IADLs need more planning and thinking. Losing IADL skills can be an early sign that someone needs support even if basic ADLs are fine.
How to Assess ADLs Quickly
You can do a simple check at home. Watch the person try to do each ADL and note whether they do it: independently, with help, or not at all. Use short notes: safe/slow/unsafe or independent/needs help/unable. Clinicians often use tools like the Katz Index or Barthel Index to score function, but your own notes are useful for appointments.
Pay attention to patterns. Is bathing the only hard task because of balance? Is dressing difficult due to arm weakness? Specific problems point to specific solutions—grab bars, a shower chair, or an occupational therapist visit.
Document changes. A one-line note each week—what was harder or easier—gives a clear picture over time. Bring that to the clinician. It helps them decide on tests, rehab, or home services.
Practical Tips to Keep or Improve ADLs
Small changes often help more than big ones. Add non-slip mats and grab bars in the bathroom, swap buttons for zippers or Velcro on clothes, use a raised toilet seat, and place commonly used items within reach. These reduce falls and make tasks doable without full assistance.
Use adaptive tools: long-handled sponges for bathing, sock aids, jar openers, and reachers. An occupational therapist can show you simple techniques to save energy and protect joints during tasks like dressing or bathing.
If you’re a caregiver, break tasks into steps, give time, and encourage the person to do as much as they safely can. That keeps skills from slipping. Schedule rest breaks and ask for help when you need it—respite care exists for a reason.
When to get professional help: sudden decline in ADLs, repeated falls, confusion while doing tasks, or heavy caregiver burden. A primary care doctor, geriatrician, or occupational therapist can create a plan with clear next steps.
ADLs are practical signals. Watch, document, and act with simple fixes first. Those small moves will protect safety and keep daily life as normal as possible.
Georgea Michelle, May, 29 2023
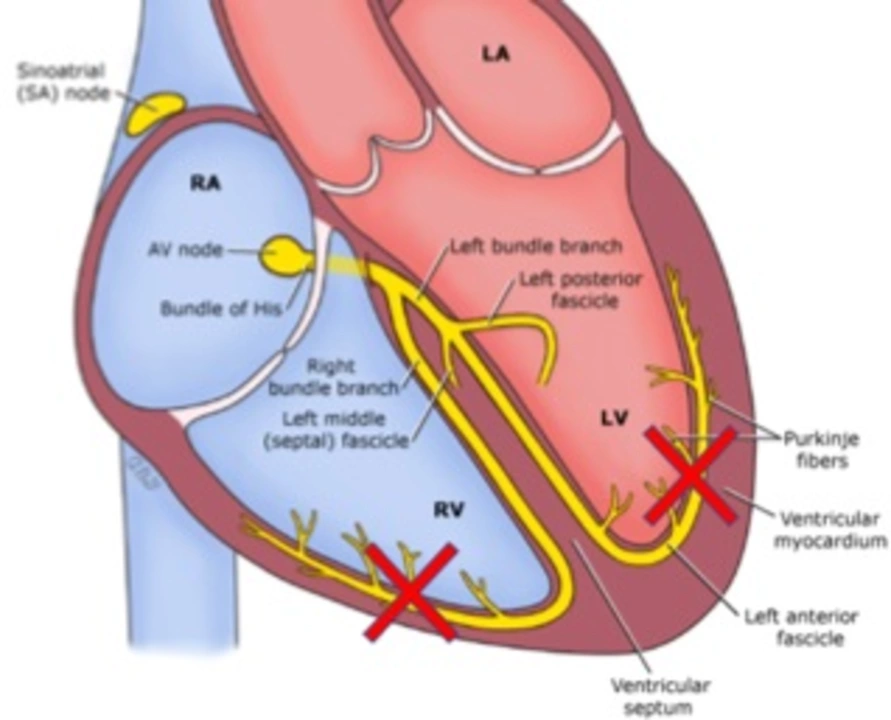
The Impact of Left Ventricular Dysfunction on Activities of Daily Living
I recently came across some information on how left ventricular dysfunction can greatly impact our daily activities. This condition weakens the heart's ability to pump blood effectively, leading to fatigue, shortness of breath, and reduced exercise tolerance. As a result, simple tasks like walking, climbing stairs, and even getting dressed can become challenging. It's crucial for individuals with left ventricular dysfunction to work closely with their healthcare team to manage the condition and maintain their quality of life. Stay informed and take care of your heart, as it plays a vital role in our overall well-being.
View More