Left Ventricular Dysfunction: Easy Guide to Symptoms and Care
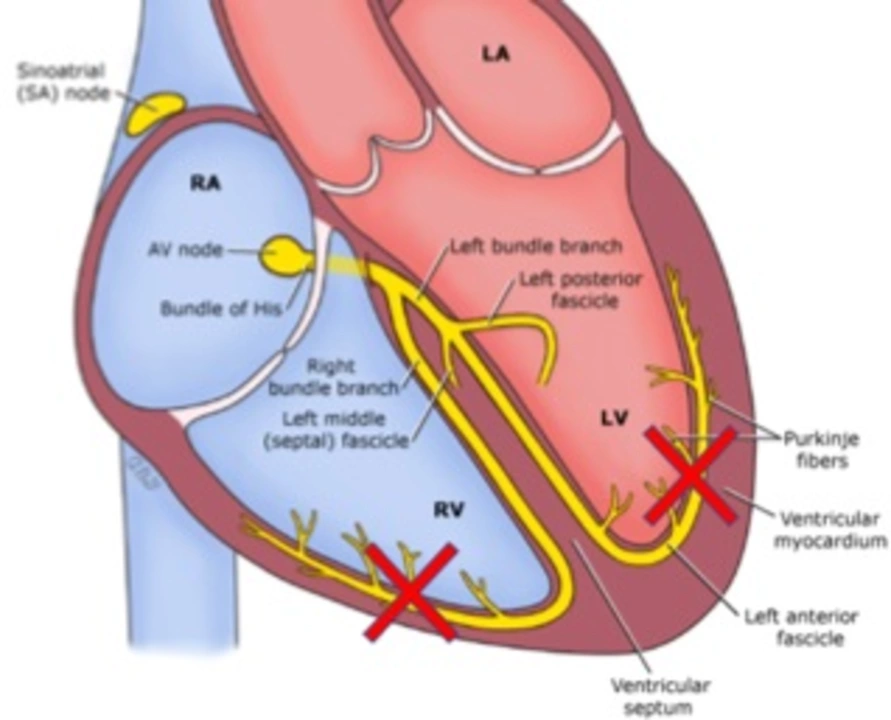
Left ventricular dysfunction means the main pumping chamber of your heart—the left ventricle—is not working the way it should. That can make you feel short of breath, tired, or swollen in the legs. It’s a common reason people end up seeing a cardiologist, but there are clear, practical steps you can take to slow it down and feel better.
How doctors diagnose it
If your doctor suspects left ventricular dysfunction they will want to measure how well your left ventricle pumps. The key test is an echocardiogram, which gives a left ventricular ejection fraction (LVEF). Numbers help guide treatment: LVEF under 40% is reduced, 40–49% is mid-range, and 50%+ is preserved.
Other useful tests include an ECG (checks rhythm), chest X-ray (looks for fluid), blood tests like BNP or NT-proBNP (markers of heart stress), and basic labs to check kidney and liver function. Sometimes doctors order coronary angiography, stress tests, or MRI if they need to find the cause—like blocked arteries or cardiomyopathy.
Treatment and daily steps
Treatment has two parts: fixing what caused the problem and protecting the heart. If coronary artery disease caused the dysfunction, procedures or medications to treat blockages may be needed. For most people, medications are the foundation: ACE inhibitors (like lisinopril), ARBs (losartan), beta-blockers (metoprolol, carvedilol), mineralocorticoid receptor antagonists (spironolactone), and newer SGLT2 inhibitors (dapagliflozin, empagliflozin) all help reduce symptoms and hospital visits. Diuretics such as furosemide are used short-term to relieve fluid overload.
Device therapy—an ICD (implantable cardioverter-defibrillator) or CRT (cardiac resynchronization therapy)—is an option when medicines don’t control symptoms or when the rhythm is risky. Your cardiologist will explain if you meet the criteria.
Daily habits matter. Cut back on salt (aim for under 2–3 grams a day unless told otherwise), track your weight daily, avoid heavy alcohol, and follow fluid limits if recommended. Gentle, regular exercise—walking or cardiac rehab—strengthens your body without stressing your heart. Keep up with vaccines like flu and COVID shots; infections can worsen heart function fast.
Know the warning signs that need urgent care: sudden severe shortness of breath, chest pain, fainting, rapid swelling, or trouble breathing while lying flat. If any of those happen, go to the ER.
Left ventricular dysfunction can feel scary, but many people improve significantly with the right mix of tests, medicines, devices, and lifestyle changes. Work closely with your doctor, ask questions about each treatment option, and get a clear follow-up plan so you can manage symptoms and stay active.
Georgea Michelle, May, 29 2023
The Impact of Left Ventricular Dysfunction on Activities of Daily Living
I recently came across some information on how left ventricular dysfunction can greatly impact our daily activities. This condition weakens the heart's ability to pump blood effectively, leading to fatigue, shortness of breath, and reduced exercise tolerance. As a result, simple tasks like walking, climbing stairs, and even getting dressed can become challenging. It's crucial for individuals with left ventricular dysfunction to work closely with their healthcare team to manage the condition and maintain their quality of life. Stay informed and take care of your heart, as it plays a vital role in our overall well-being.
View More